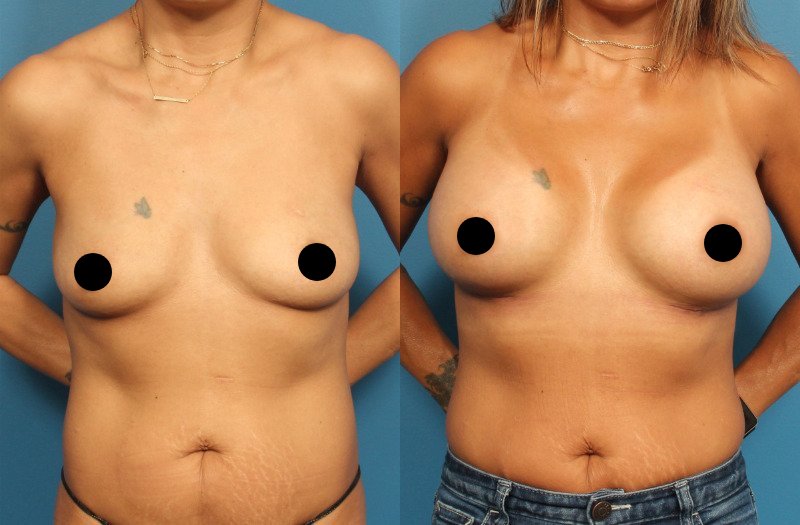
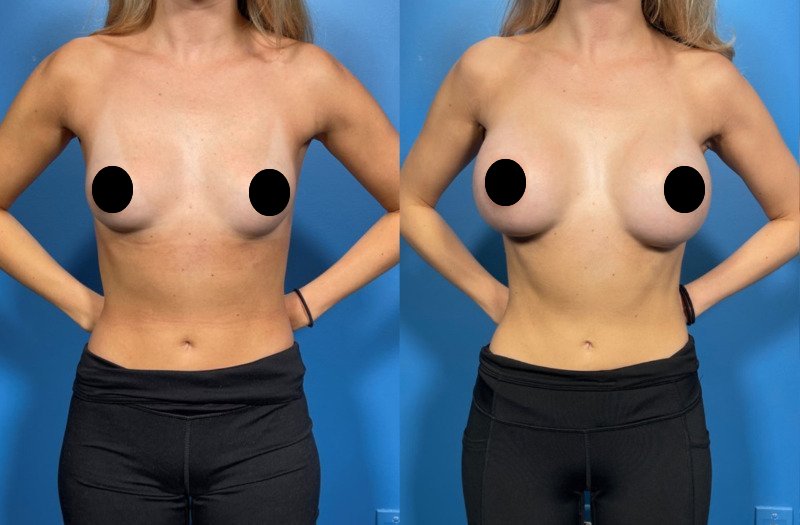
Whatever your personal reasons, we’re here to help you explore the possibilities and achieve the results that are best for you and your body. Whether you wish to increase the size of your breasts or improve their shape, breast augmentation is an enormously satisfying procedure for most patients.
Our team is committed to your understanding of what breast augmentation in Cary, NC involves and the options that are available to you. CARE Plastic Surgery is a state-of-the-art facility and Dr. Coan is one of the best plastic surgeons in the nation for breast surgery. You have found the right surgeon! Let’s learn more about the subject.
What is Breast Augmentation?
Breast augmentation is a plastic surgery procedure performed to enhance the size and shape of the breasts. This is most often achieved through the placement of a breast implant. The main goal of this procedure is to enhance a patient’s natural proportions to create a more pleasing breast profile. This may be achieved by adding balance to the body, restoring breast fullness after pregnancy, addressing asymmetry, and more.
Candidates for Breast Augmentation Surgery
You may be an ideal candidate for breast augmentation if you are physically healthy, are not pregnant or breastfeeding, have breasts that are fully developed, and have realistic expectations regarding the results of this procedure. The best way to determine if this procedure is right for you and your personal goals is to schedule a consultation appointment at our Cary, NC office today.
What are the Choices Available to You for Your Breast Augmentation?
In the past, surgeons often made all the choices for their patients. This led to a high revision rate and many women wished they had more control over the process and results. At CARE, we believe the best choices are those made together – surgeon and patient. Achieving your aesthetic goals and improving patient self-confidence are our ultimate goals.
A consultation with our surgical team will cover every detail about your treatment options. This includes what cup size you hope to achieve, the breast shape you desire, and the type of implant you want. There are options to add a breast lift to your augmentation if sagging breasts are a concern along with volume. Additionally, some patients with enough existing breast tissue may benefit from breast lift procedures alone.
Breast implants are highly customizable. Most women are aware that they can help choose the size of their implants as well as the implant type. There are other decisions that must be made as well, including:
- The shape of the implant
- Profile of the implant (the amount that the breast projects outward from the chest in profile)
- The texture of the implant
- Location of the incision and scar
Read our blog ”Which Breast Implant Shape is Best for You?” to learn more. With all the available choices for your breast procedure, no wonder people get confused! Board-Certified Plastic Surgeon Dr. Coan is an expert in breast augmentation surgery and will help guide you through the process.
Breast Implant Placement Options
When choosing to undergo breast augmentation with implants, the placement of the implants must be considered. Dr. Coan can place your implants over or under the muscles of your chest. The implant placement that is right for you will depend on your individual anatomy and personal aesthetic goals.
Subglandular Placement
Subglandular placement involves placing the breast implant in front of the chest muscle but behind the glandular breast tissue. This technique is ideal for placing larger breast implants. However, implants may feel less natural.
Submuscular Placement
Submuscular implants are positioned behind the chest muscle wall. This placement can achieve a more natural appearance. However, this technique is more invasive, and therefore recovery time may be longer.
Types of Implants for Breast Augmentation
Along with implant placement, you must also consider which type of implant is best for you. There is an array of different implant options available on the market today, including saline, silicone, and gummy bear.
Saline Implants
Saline breast implants are made of a silicone shell filled with a sterile saltwater solution. They are FDA-approved for use in women aged 18 and older. If an implant leaks, the implant would collapse, and the saline would be naturally absorbed and expelled from the body. Although a popular option, it is not offered at CARE Plastic Surgery.
Silicone Implants
Silicone breast implants are a popular and FDA-approved option for women aged 22 and older, offering a natural look and feel that closely mimics breast tissue. These implants consist of a silicone shell filled with a cohesive silicone gel, providing a soft and realistic texture that many women prefer over saline alternatives. One of the key advantages of silicone implants is their durability and stability. In the rare event of a rupture, the cohesive nature of the gel helps maintain the implant’s shape, preventing collapse and minimizing the risk of noticeable changes in breast appearance. This unique characteristic contributes to the long-lasting aesthetic results that many patients desire. While routine check-ups are recommended to ensure optimal implant health, the overall safety and satisfaction rates for silicone implants remain high, making them a trusted choice for breast augmentation and reconstruction procedures.
Motiva and Natrelle Implants
Dr. Coan offers breast augmentation with both Natrelle and Motiva implants, including the popular Natrelle “gummy bear” silicone option. In most cases, he recommends round implants placed beneath the chest muscle through an incision hidden in the breast fold, which helps limit visible scarring. Since every patient’s goals and anatomy are unique, Dr. Coan reviews all available techniques—such as implant type and incision location—during the consultation to create a personalized surgical plan. To help patients understand their options, it’s important to look more closely at the unique benefits of both Natrelle and Motiva implants.
Motiva breast implants represent the next generation of silicone gel breast implants, designed with advanced technology to improve both safety and aesthetics. Developed by Establishment Labs, these breakthrough implants are FDA-approved in the United States and supported by three-year clinical data, demonstrating high patient satisfaction and a reduced risk of complications, including capsular contracture. Motiva implants are engineered to closely mimic the look and feel of natural breast tissue, offering patients seeking breast augmentation a natural appearance and long-lasting results.
Natrelle Implants
Natrelle® breast implants, developed by Allergan Aesthetics, are FDA-approved silicone gel implants known for their safety, versatility, and natural-looking results. These implants are a type of silicone breast implant known for their cohesive gel filling, which helps them maintain shape and provide a natural feel. Because the gel is thicker than that found in traditional silicone implants, they are often called “gummy bear” implants, as they retain their form even when cut. Patients often choose Natrelle implants for their soft, natural look, durability, and wide range of shapes and sizes, allowing for a highly customizable breast augmentation result.
Breast augmentation surgery is performed under general anesthesia in our outpatient surgical center. Dr. Coan will make an incision in an easily concealed spot, usually under the breast fold or around the nipple-areolar complex. He will then place breast implants under or over the pectoral muscles in the chest. Surgery can take 1-3 hours, depending on whether any additional procedures are added.
Recovering From Breast Augmentation Surgery
Following breast augmentation, you will need to have a trusted friend or family member drive you home and stay with you for at least a few hours. You can expect to walk around on your own a few hours after surgery.
Soreness is to be expected for the first week after surgery, and you will need to limit strenuous activities for 2-4 weeks. Pain medication can be prescribed to help with any discomfort. You will also be asked to wear a surgical bra to support your new breast contour and prevent swelling. It is crucial to follow Dr. Coan’s aftercare instructions for optimal results. Do not hesitate to reach out with any questions or concerns you may have following your surgery.
What to Expect Following a Breast Augmentation
While the results of a breast augmentation will be noticeable right away, the final results may take a couple of weeks to become apparent as swelling subsides and the breasts settle into place. Incisions may take several months to a couple of years to fully fade.
Once swelling has gone down and incisions have healed, patients can enjoy fuller, more shapely breasts. Many women report a boost in self-confidence and the ability to wear clothing more confidently.
Breast implants are not meant to last a lifetime, and therefore will need to be replaced eventually. We recommend visiting your plastic surgeon for an annual exam to evaluate your implant integrity. Breast implant exchange after some time can help to restore a more youthful breast contour.
Alternatives to Breast Augmentation
While breast implants are a popular option for improving breast size and shape, fat transfer is an alternative option. This involves removing fat through liposuction from a certain area of the body such as the stomach or thighs and re-injecting it into the breast to add volume.
This option may be right for individuals who are happy with their breast shape but are looking for a small boost in volume, have some extra fat on the stomach, hips, or thighs, and prefer natural fat transfer over implants.
Frequently Asked Questions
Are breast implants under warranty?
Breast implant warranties vary depending on the company or manufacturer. In general, there is a 10 year warranty against implant leaking or rupture. This is a fairly low occurring event, at approximately 6% at 10 years. If it occurs, the implants are replaced, and the company covers a portion of the surgical costs. If the implants leak or fail after 10 years, although the surgical costs are not covered, the cost of replacement implants are covered for life. In the event a patient develops capsular contracture (a formation of excess scar tissue around the implant), surgical costs are not covered, but replacement implants are covered if it occurs within the first 3 years.
Can breast implants cause pain years later?
One risk of breast implants is the development of capsular contracture. Capsular contracture is the hardening of the thin scar tissue that surrounds the implant. In moderate to severe cases, capsular contracture can cause a tightness, firmness, or painful feeling in one or both breasts. Treatment options for capsular contracture include medical management with medications and possible implant removal and/or exchange. At CARE Plastic Surgery, we take every measure to reduce the overall risk of capsular contracture. We are proud to say that Dr. Coan’s rate is about one-third of the national average.
Can breast implants last 30 years?
Yes, with today’s silicone implant technology, breast implants can last decades. At CARE Plastic Surgery, we offer Allergan Natrelle silicone implants that include a lifetime warranty. At 10 years after implantation, the rate of implant leaks and/or ruptures is considerably low at about 6%. We recommend patients receive MRIs to evaluate the integrity of the implant, as this is the only way to detect a leak or rupture in a silicone implant.
Can fat be transferred to breasts?
Yes, you can augment the breast with use of an implant or fat grafting. At CARE Plastic Surgery, we offer a variety of surgical procedures, including fat transfer to the breasts. Depending on your desired aesthetic goals, our double-board certified plastic surgeon may recommend utilizing a breast implant or fat grafting to the breasts. Oftentimes, fat transfer can achieve a more natural aesthetic and may be a suitable option for patients seeking minimal volume increase.
Can I move my arms after breast augmentation?
You will be able to move your arms after breast augmentation surgery. Depending on the patient, we may recommend avoiding certain movements, such as raising your arms above your head, for a short period of time after your procedure. We discourage patients from lifting anything exceeding 20 pounds, or participating in any activity causing an increase of heart rate and blood pressure for approximately 6 weeks after surgery.
Can you breast feed after breast augmentation
There is no proven evidence indicating an implant would significantly impact a woman’s breastfeeding ability. Relevant factors that can impact a woman’s ability to breastfeed include the amount of existing breast tissue, age, and genetics.
Do breast implants cause autoimmune disease?
There is no direct evidence supporting that silicone implants are a causal factor for autoimmune disorders. While patients may develop autoimmune disorders over the course of their lifetime, along with other disorders or conditions, there is no clinical data indicating silicone implants cause autoimmune disease. The breast implant is considered one of the most clinically studied medical devices on the market.
Do breasts sag after breast augmentation?
Breast implants serve to solely make an ideal-shaped breast larger. Implants do not address nipple position or breast shape. Implants are not \u201canti-gravity\u201d devices, meaning breasts with implants will continue to age similarly to large breasts without implants. Implant position can be influenced by weight fluctuations, pregnancy, hormonal changes, and more. Our double-board certified surgeon, Dr. Coan, will help you decide if a breast lift is right for you prior to surgery.
Do you have to replace breast implants every 10 years?
Some people may mistakenly compare medical breast implants to car tires, and believe they need to be \u201crotated\u201d or changed periodically. Many breast implant manufacturers offer a breast implant warranty and the Natrelle brand breast implants for silicone gel offer a lifetime replacement warranty and a 10-year warranty on capsular contracture. Silicone gel breast implants that are FDA approved are designed to serve as lifetime medical devices. It is common for many patients to enjoy their implants for 15-20 years or more with proper maintenance. Patients may decide to replace their implants for many reasons, including ruptures, after breastfeeding or changes in aesthetic desires. Because implants are not an \u201canti-gravity\u201d device, a patient’s breasts may change due to weight fluctuations, pregnancy, or hormonal changes.
Does getting breast implants make you gain weight?
Technically, minimal weight gain is to be expected when getting breast implants, but it will not be noticeable, nor should it have an impact on your decision to go through with breast implants.
How do I know if my breast implant is leaking?
It is fairly easy to detect a leak in saline implants. Patients will notice a physical change in the appearance of the implant as it subsequently deflates. Although the leak rate is relatively low, the only way to detect a leak in a silicone implant is with an MRI.
How painful is breast augmentation recovery?
While every patient is unique, many patients commonly describe the post-operative experience as sore rather than painful. The majority of patients find comfort after surgery when following the recommended pain management and medication regimen. Many patients at CARE Plastic Surgery report feeling back to their \u201cnormal selves\u201d within a week. Most patients only take pain medicine for 2-3 days. The vast majority of our patients only take non-steroidal anti-inflammatories after the first day.
Is there an alternative to breast implants?
Yes, an alternative way to enlarge the breasts would be through liposuction and fat transfer. This is a great option for patients wanting a more natural appearance.
What is the difference between a breast augmentation and breast implants?
Breast augmentation is any procedure that serves to increase the size of the breast. A breast can be enlarged by means of fat transfer or a breast implant device.
Are silicone or saline implants better?
Silicone implants provide a more natural appearance, less chance of visible rippling, and have a lower implant rupture rate. With a rupture in saline implants, there is a subsequent abrupt deflation, which results in a noticeable change in appearance and requires implant replacement.
Do you use saline or silicone implants?
At CARE, we offer all types of implants but recommend Allergans Natrelle silicone gel implants. The Natrelle breast implants are considered to be the gold standard for many reasons, including a lifetime replacement warranty and a ten-year implant replacement warranty on capsular contracture. Most patients appreciate the substantial advantages of these implants over the small cost differential associated with the less expensive saline implants.
Can you prevent capsular contracture?
There are certain measures that can be taken to ensure the lowest risk of capsular contracture. Some factors are patient-dependent and can increase the risk, such as frequent UTIs, sinus infections, and recurrent dental problems. At CARE, we implement all the best practices to minimize your overall risk of capsular contracture. Dr. Coan uses silicone implants placed below the muscle using an incision at the infra-mammary fold unless otherwise indicated.
What is capsular contracture?
Capsular contracture is a rare but serious risk associated with breast augmentation surgery. After surgery, a thin layer of internal scar tissue forms around the implant. In capsular contracture, the scar tissue thickens and hardens, leading to a conformational change of the breast. In addition to a shape change, the breast can feel tight and/or painful. Treatment involves implant removal and/or exchange, and the procedure may require a capsulectomy.
What is the risk of capsular contracture?
The national average risk of developing capsular contracture after a breast augmentation is around 10-12%. At CARE Plastic Surgery, our rate is around 3-4%. Dr. Coan performs every measure possible to mitigate this incidental risk including often placing the implant under the muscle and often using a Keller Funnell to mitigate implant contamination.
What are the restrictions after breast augmentation?
During the first two weeks after surgery, we advise patients to take it easy to avoid complications, such as bleeding or bruising. Additionally, we encourage patients to sleep in a relined position during this time to help with overall swelling. We instruct our patients to avoid exercise and any activities that will increase heart rate or blood pressure for 6 weeks following surgery. This includes no pushing, pulling, or lifting objects over 20 lbs. Also, patient should avoid baths or swimming until all incisions are healed (typically around 6-weeks post-op).
Do you have to wear a bra 24/7 after breast augmentation?
We recommend our patients wear a compression bra for 6 weeks after surgery, including while sleeping at night. Patients may take it off for showering, laundering, and breast massage.
What activities can you not do with breast implants?
Our patients are instructed to avoid exercise and any activity that will increase heart rate or blood pressure for 6 weeks following surgery. At 6 weeks, our patients are cleared to resume any and all activities. We want our patients to \u201cforget\u201d they had surgery and enjoy their lives and new bodies! We often tell our patients with military background that they can jump out of a plane if they desire.
What happens at my initial consultation?
At your initial consultation, you will meet face-to-face with our double-board certified plastic surgeon, Dr. Brian Coan. He enjoys spending time getting to know you as an individual, discussing your lifestyle, aesthetic goals, and questions/concerns. After performing a brief examination, he will provide his expert recommendations based on your anatomy and goals. You will then participate in a sizing session, allowing you to physically try on various implants to see what volume range you like on your frame. Our patients really enjoy this part of the consultation, and oftentimes they try on fitted shirts and take selfies!
Is a breast augmentation covered by Insurance?
Most breast augmentations are considered cosmetic procedures, which are often not covered under insurance. At CARE Plastic Surgery, we are out-of-network with all insurance companies.
What are the different types of breast implants?
There are many different types of implants on the market. At CARE, we offer Allergan’s Natrelle silicone implants. Silicone implants are considered to be the gold standard for many reasons. Compared to saline implants, silicone implants have a lower chance of visible rippling, reduced risk of capsular contracture, and lower leak/rupture rate. With a rupture in saline implants, there is a subsequent deflation which requires implant removal. Additionally, patients may find that silicone implants feel more natural. There are also hundreds of different silicone implants in the Allergan Natrelle portfolio, with various projections and gel types.
What should I expect after a breast augmentation?
While every patient is different, many patients commonly describe the post-operative experience as sore rather than painful. The majority of patients find their pain to be well-controlled when following the recommended pain management regimen. Patients often report feeling back to their \u201cnormal selves\u201d within a week. Most patients may only take pain medicine for 2-3 days. The vast majority of our patients only take non-steroidal anti-inflammatories after the first day. It is important to remember that final results are judged at 3 months post-op, so your breasts will continue to undergo subtle changes throughout this time.
How long does a breast augmentation take?
Breast augmentation is considered an outpatient procedure. The actual procedure time takes about 45 minutes, depending on if other procedures are being performed at the same time (i.e. breast lift, nipple reduction, etc.). This does not include total prep and anesthesia time. Patients and their caregivers can expect to be at the office about 2-2.5 hours from start to finish.
What kind of scars will I have?
Depending on a patient’s starting point, anatomy, and aesthetic goals, Dr. Coan may recommend different incisions to accomplish the best aesthetic outcome. For a breast augmentation with no simultaneous breast lift, the best incision to utilize is located in the inframammary fold, or natural crease at the bottom of the breast. This is associated with the lowest risk of capsular contracture. Other possible incisions used include a periareolar incision with a circle around the areola, or a \u201clollipop\u201d incision with a circle around the areola and a vertical incision on the front of the breast. These are associated with breast lift procedures. Scarring can depend on a multitude of factors, including the body area. Breasts tend to heal quite well, but scarring is also patient-dependent. Scar quality can depend on genetics, skin quality, complexion and skin type, and lifestyle habits (i.e., degree of sun exposure, smoking). The best treatments for optimal scarring are time and avoiding sun exposure. The appearance of scars is typically best at about 1 year after surgery. We also recommend Biocorneum, which is a silicone-based scar gel containing SPF. This is the only FDA-approved scar treatment on the market, and we encourage our patients to incorporate this once all incisions are healed.
How many post-op appointments will I have?
We commonly see patients the day after surgery, 2 weeks post-op, 6 weeks post-op, and 3-months post-op. Some of these can be conducted virtually if patients drive from a long distance. Depending on the patient, we will typically recommend the day 1 appointment, 2-week post-op, and 3-month post-op appointments be done in-office. However, we are always happy to see patients at any time if there are questions and/or concerns. Dr. Coan and our clinical team are always readily accessible to our patients.
How much does a breast augmentation cost?
Total cost of breast augmentation depends on a few factors, including other simultaneous procedures (i.e. breast lift) and implant type. Ultimately, Dr. Coan and our team want to provide you with the best possible result. Here at CARE Plastic Surgery, our patient care coordinators will work with you to accomplish your aesthetic goals. We offer a variety of financing options, including CareCredit, Alphaeon Credit, and PatientFi. Additionally, we accept several methods of payment, including cash, check, cashier’s check, and most major credit cards.
How does breast augmentation with fat transfer differ from implants?
Breast augmentation with fat transfer and breast implants are two different techniques used to enhance breast volume. Fat transfer uses liposuction to remove fat from areas like the abdomen, flanks, or thighs, which is then purified and injected into the breasts. Implants involve placing a silicone or saline device to increase breast size. The primary differences include the materials used, the total procedure time, the range of achievable volume increase, and incision locations. Both options have their own advantages and limitations, depending on the patient’s anatomy and goals.
Am I a good candidate for breast fat transfer surgery?
Good candidates for fat transfer breast augmentation are individuals in overall good health, with realistic expectations, and adequate excess fat available for harvesting. It is typically best suited for those seeking a more modest increase in breast size. A consultation is necessary to determine whether fat transfer or breast implants would best align with your aesthetic goals and body type.
How long do results from fat transfer breast augmentation last?
Results from fat transfer can be long-lasting, but it’s important to know that not all transferred fat will survive — typically about 60-80% remains after the healing process. Some of the transferred fat is naturally reabsorbed by the body in the first few months. The fat that does successfully establish a blood supply will remain permanently. Final results are usually seen and evaluated at 3 months post-op, and like all procedures, results can be influenced by factors such as weight fluctuations, aging, and lifestyle.
What is recovery like after breast augmentation with fat transfer?
Recovery after fat transfer breast augmentation involves healing at both the donor sites (where fat is removed) and the breasts (where fat is injected). Patients can expect mild to moderate swelling, bruising, and soreness in these areas during the first 1-2 weeks. A compression garment is worn for 6 weeks to support healing and minimize swelling. While light daily activities can usually be resumed within a few days, it is important to avoid any exercise or activities that could elevate heart rate or blood pressure for 6 weeks to minimize risk of complications. Recovery experiences may vary slightly based on individual factors and any combined procedures.
Can fat transfer be combined with other breast procedures?
Yes, fat transfer can be combined with other breast procedures. Some patients may pair fat transfer with a breast lift to increase upper pole fullness and reshape the breasts. Your board-certified surgeon can customize a plan based on your anatomy and aesthetic goals.
Meet Dr. Coan
Award-winning, nationally renowned, double board-certified Plastic Surgeon and a member of the distinguished Fellow of the American College of Surgeons (FACS).
A monthly medspa membership, currently by invitation only, for exclusive pricing on Botox®, fillers, skincare, CoolSculpting® & skinCARE products. Learn More
Real Testimonials
I adore Dr. Coan & his whole staff. They are kind, warm, fun, & helpful. I trust Dr. Coan wholeheartedly. He is always honest with me, and would never sell or recommend a procedure that is not right for me. I love my office visits and look forward to going! Dr. Coan is my forever.
- Verified Care Plastic Surgery Patient
Beauty of the Ages
Find out which procedures are the best fit, select your age to see recommendations!
Patient Stories
Learn about our amazing patient experience and see what you can expect from the CARE team.
I am so happy and I feel so confident!
Additional Treatments to Consider
Procedures can be combined to maximize your benefits and target multiple concerns in one treatment. Customize your procedure at CARE with the following treatment options.
New Patient Resources
Need to know more about our process? Check out a few of our blog posts below.
First Steps of Breast Augmentation
Read
Breast Augmentation and Breast Lift: What’s the Difference?
Read
Dr. Brian S. Coan is an award-winning, nationally renowned, double board-certified Plastic Surgeon and a member of the distinguished Fellow of the American College of Surgeons (FACS). With over a decade of experience, his commitment to excellence has transformed countless lives.